What’s the Relationship Between Intermittent Fasting and Eating Disorders?


- Intermittent fasting is a popular health trend, but it shares similarities with disordered eating behaviors, and can be a risk factor for developing an eating disorder..
- Experts don’t recommend intermittent fasting for people with a current eating disorder, those in eating disorder treatment, or those who’ve had a past eating disorder.
- Intermittent fasting is also a risky choice for anyone who may be vulnerable to developing an eating disorder, as it could be a trigger for those predisposed.

Diet culture is omnipresent in our lives, but it’s always shape-shifting. One of the more recent ways that diet culture has shown up is with the trend of intermittent fasting, or not eating for certain hours of the day.
Over the past few years, countless people have jumped on the intermittent fasting bandwagon, usually out of a genuine desire to improve their health. But the reality is that intermittent fasting itself can be a disordered eating behavior, and can lead to other problematic and unhealthy habits.
Read on to learn more about the risks and benefits of this practice, the relationship between intermittent fasting and eating disorders, whether it’s safe for those in recovery, and more.
What is intermittent fasting?
Intermittent fasting is one of the most widespread eating approaches in the United States, surpassing the ketogenic (keto) diet in popularity. Instead of setting rules about what types of foods you can and can’t consume (like limiting carbs with keto), intermittent fasting involves rigid rules about when—rather than what—you eat.
“There’s a length of time in the day when a person chooses to eat, and a length of time they choose to fast,” explains dietitian Lauren Chaffin, RD.
“There are several methods with varying time ranges,” she says, “such as a 16-hour fast with eight hours of eating, or fasting days, in which a person may cut way back on their caloric intake for five days, and then eat in a surplus for the remaining two days of the week.”
According to Equip dietitian Rui Tanimura, RD, other intermittent fasters may have one large meal per day and avoid all meals and snacks otherwise, which is sometimes referred to as OMAD (“one meal a day”) on social media and elsewhere. Exactly how intermittent fasting looks will vary from person to person, but the basic principle is the same: limiting food intake during set periods and allowing unrestricted access to food during other periods.
Are there proven benefits of intermittent fasting?
Proponents claim that intermittent fasting has several significant health benefits. These include increasing lifespan, improving conditions associated with inflammation (like Alzheimer’s), preventing cancer, and improving heart health. Weight loss is also high on the list of touted benefits.
“Supporters claim that it’s an effective approach to control or change weight, improve metabolism, and to prevent overeating,” Tanimura says.
Some studies support the benefits of intermittent fasting—but they don’t show direct causation. In other words, the studies might show that intermittent fasting is associated with lower blood pressure, but the research doesn’t indicate whether one causes the other of if there’s a third factor driving the association (for example, maybe people who stick to an IF diet are more likely to take certain blood pressure-supporting supplements).
This is an example of how correlation doesn’t equal causation. Another way to think about this concept is through a famous example. Ice cream sales and shark attacks are correlated (associated) with each other. But eating ice cream clearly doesn’t cause shark attacks. Instead, ice cream sales go up in summer because it’s a cooling treat in hot weather. And more people swim in the ocean in summer. Therefore, more shark attacks occur during the season.
The existing research on intermittent fasting and eating disorders also lacks data from which we can make any evidence-based recommendations about the trend. “Intermittent fasting, just like any other fad diet, has far-reaching claims attached to it,” Chaffin says. “The problem is, the research on intermittent fasting has been done almost exclusively in a lab on animals.”
For example, one study showing a link between intermittent fasting and longevity was conducted with fruit flies, and another was conducted on mice. Research that associated intermittent fasting with Alzheimer’s improvement or cancer prevention also used animals.
Chaffin says the reason for the limited number of human trials is because of the restrictive nature of intermittent fasting. “It’s not sustainable,” she explains, “so many people drop out or are unable to complete the trial.”
Some human studies show positive associations between intermittent fasting and cardiovascular risk factors like diabetes and hypertension. Yet they are too small and too short in duration to draw conclusive recommendations.
“There’s just simply no way to know the benefits versus risk factors without looking at a large population of people over a long period of time,” Chaffin says. “The studies that do show ‘improvements’ only last somewhere between one to 12 weeks total. Compared to a lifetime, it’s a tiny blip of time.”
When considering what the research says about weight loss, the story remains much the same. Studies are too small and too short to prove the diet “works” in the long run. “Most intermittent fasting research continues to need more longer-term outcomes,” Tanimura says.
A recent randomized clinical trial examined the effects of intermittent fasting on weight loss for 12 weeks. The study showed no differences in weight loss between intermittent fasters and consistent eaters.
Like all other restrictive diets, intermittent fasting comes with several potential side effects. These include extreme hunger, fatigue, insomnia, nausea, and headaches. Plus, research shows that dieting can lead to eating disorders.
Is fasting bad for you? The potential risks and side effects of intermittent fasting
Like all other restrictive diets, intermittent fasting comes with several potential side effects.
Physical side effects
The potential physical dangers of intermittent fasting include:
- Dehydration: Fasting windows allow for drinking no-calorie beverages, but research indicates reports of dehydration.
- Digestive issues: Fasting can cause constipation, gas, and bloating—and prolonged fasting is associated with gallstones and gallbladder attacks.
- Dizziness: More than half of participants in one study reported this side effect.
- Extreme hunger: No surprise here, but fasting windows can lead to cravings.
- Fatigue: Fasting windows can leave you feeling low energy.
- Headaches: Almost two-thirds of participants in one study reported headaches.
- Nausea: Feeling queasy during fasting windows is also a reported side effect.
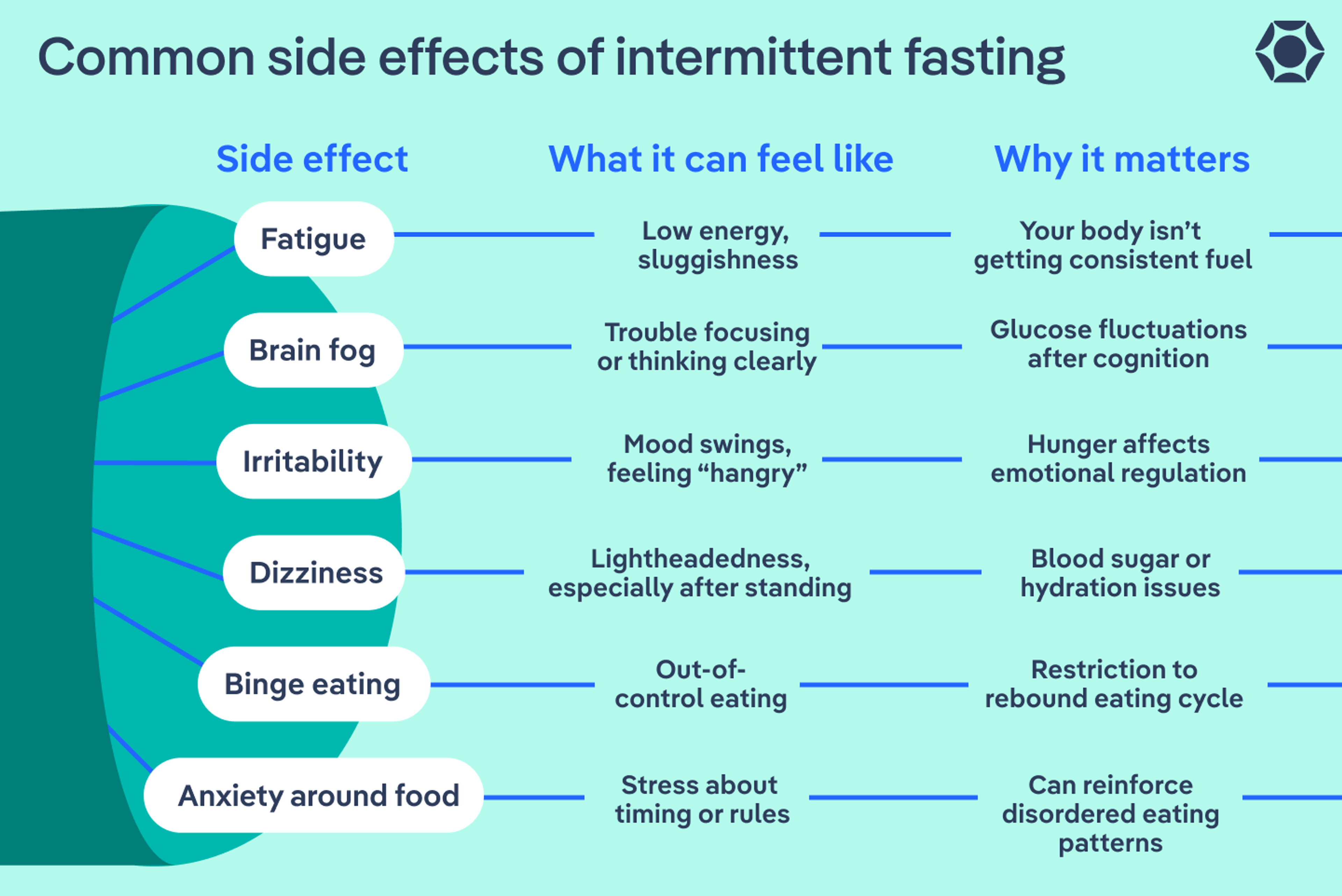
Mental and emotional side effects
Additionally, intermittent fasting risks include some potential negative psychological impacts. The main one is mood swings. In one study, more than half of participants reported mood swings with intermittent fasting. This may be because feeling hungry can lead to irritability, or that “hangry” feeling.
Eating-disorder-related risks
Research also shows that dieting is one of the biggest risk factors for developing an eating disorder. And intermittent fasting specifically can lead to disordered eating behaviors, as well as increased risk for developing a full-blown eating disorder, which we unpack in more detail below.
The extreme hunger during fasting windows can lead to uncontrolled or binge eating. Likewise, the feeding window could also drive binge-eating behaviors, worsen restrict-then-binge cycles, or drive restriction in general.
Fasting can also lead to a negative energy balance, where you are taking in fewer calories than what you are burning. This can be an eating disorder trigger.
Is intermittent fasting an eating disorder?
In short, no, intermittent fasting is not an eating disorder. However, all restrictive diets—including intermittent fasting—can be considered a form of disordered eating. This is a term used to describe a vast range of unhealthy eating behaviors that don’t necessarily constitute a full-blown eating disorder.
Any sort of rigid food rules, like the ones necessary to maintain intermittent fasting, foster unhealthy behaviors around food and a hyper-fixation on food and body size. Intermittent fasting may also sever the natural connection between our minds and bodies.
“When we use external factors, like the time, to tell us when we can and can’t eat,” Chaffin explains, “we’re telling our bodies that they are not to be trusted and that the cues and signals they give us can be ignored.”
Intermittent fasting itself is not an eating disorder. But it does encourage several behaviors associated with eating disorders.
One year-long study of young adults and teens of all genders showed a significant link between intermittent fasting and eating disorder behaviors like compulsive exercise, vomiting, and severe food restriction.
Gretchen Wallace, RD, points out that the very structure of intermittent fasting lends itself to another eating disorder behavior: binge eating. “Intermittent fasting involves restriction for a large part of the day followed by a food free-for-all, which could look or feel like a binge,” she explains.
Rigid rules and the behaviors described above are often symptoms of eating disorders. But not all intermittent fasters will experience disordered eating behaviors or thoughts.
However, “that can change if the diet is followed for a long period of time,” Wallace says. “You won't find intermittent fasting listed as a diagnostic criteria in the DSM. But it can quickly shift from being an experiment for your health to a disordered relationship with food—or a full-blown eating disorder.”
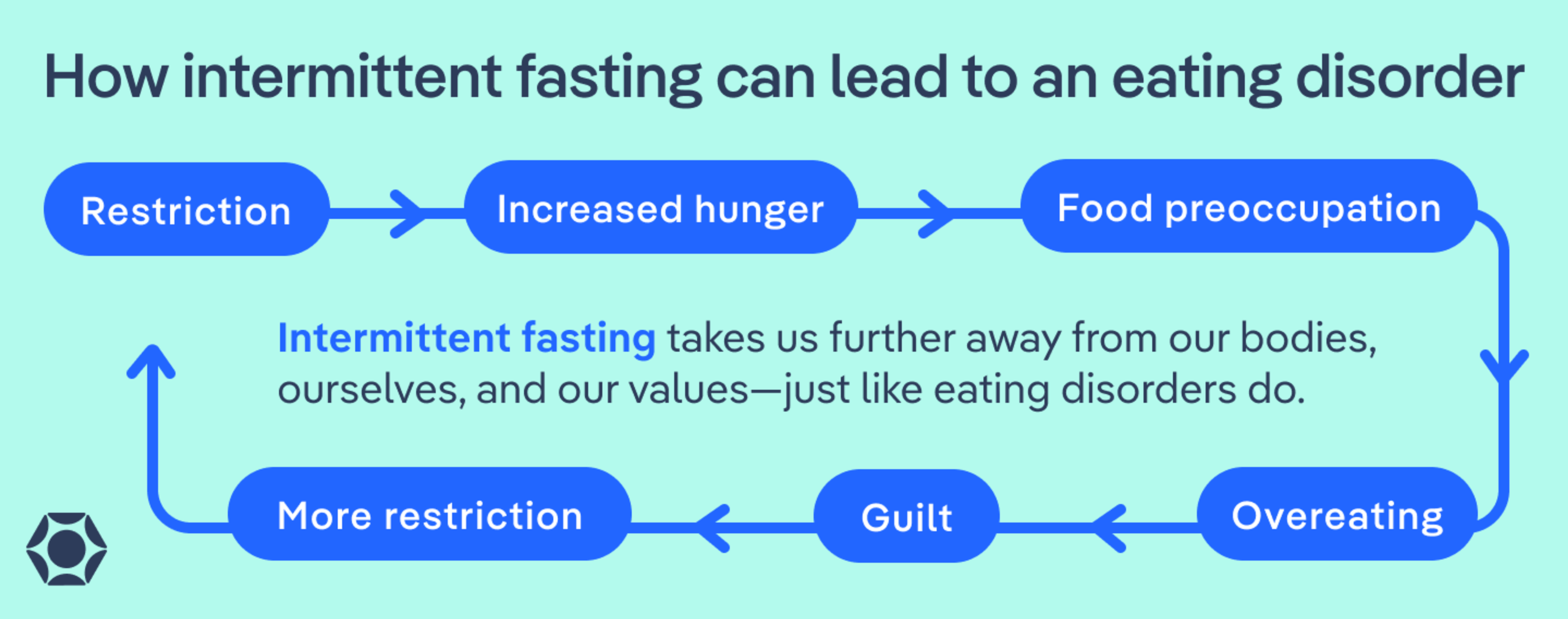
How intermittent fasting can lead to an eating disorder
As Wallace explained, intermittent fasting has the potential to lead to an eating disorder over time. What may start out as a genuine attempt to experience health benefits can become a slippery slope that descends into disordered eating patterns.
These patterns often build off one another and become more extreme. Remember, any restrictive eating pattern carries psychological and physical health risks. That’s why telling the difference between a diet and an eating disorder can be difficult.
“Your body doesn’t understand that this ‘famine’ is self-inflicted. So it’s going to be on high alert to increase its ability to survive and find food,” explains Equip Nutrition Director Erin Reeves, RD.
“You might be thinking about food more or feel more out of control when you do eat,” she adds, “because your body can’t trust there won't be a famine again.” Tanimura tried intermittent fasting herself. She says it was one of the behaviors that ultimately led to her eating disorder diagnosis.
“It is an extreme behavior that can likely trigger other eating disorder behaviors or attitudes, such as body dissatisfaction, a desire to adopt severe restriction methods, binge eating, low self-esteem, food rules, and attempting to ignore and suppress hunger cues,” she says.
Learning about the Minnesota Starvation Experiment can help illuminate why fasting can have this effect.
How can you tell when intermittent fasting is becoming disordered?
If you or a loved one has been engaging in intermittent fasting, you might be concerned about disordered eating. If you answer yes to one or more of the following questions, fasting practices could be a concern.
- You feel guilty, ashamed, or anxious if you eat outside the fasting window.
- You keep extending your fasting window or adding more rules.
- You ignore hunger, fatigue, dizziness, or feeling unwell.
- You use fasting to “make up for” eating.
- You think about food most of the day.
- You binge or feel out of control when you finally eat.
- Your social life, mood, concentration, or all three are suffering.
For further insight, you can take the short and clinically validated Equip Health eating disorder screener.
Is intermittent fasting safe for people in eating disorder recovery?
Experts do not consider intermittent fasting to be a safe practice for those recovering from an eating disorder. This applies whether you’re freshly in recovery or have been recovered for many years.
The practice could lead to a relapse. Think of it like this: attempting intermittent fasting while in eating disorder recovery would be like trying to drink one glass of wine a day when you’re in recovery from alcohol use disorder.
Plus, the principles of intermittent fasting and eating disorder recovery are in direct conflict with each other.
“The components of intermittent fasting do not align with the pillars of eating disorder recovery, such as creating consistent meal and snack times every two to four hours, feeling and honoring our hunger and fullness cues, and removing debilitating food rules,” Tanimura explains.
What’s more, intermittent fasting and other diets are externally driven, taking us further away from our bodies, ourselves, and our values—just like eating disorders do.
“I would never recommend dieting to a person in recovery. And intermittent fasting is going to be particularly triggering due to its similarity to disorders like anorexia, binge eating disorder, bulimia, and OSFED,” Wallace says.
“If you’re in recovery from an eating disorder and are interested in the alleged health benefits of intermittent fasting,” Wallace continues, “I suggest talking to an eating disorder clinician about how to incorporate health-promoting behaviors into your recovery rather than pursuing a diet such as intermittent fasting.”
What are the alternatives to intermittent fasting?
The healthiest way of eating is one that supports your mental, emotional, and physical well-being, and helps you live in alignment with your core values.
One specific eating framework, called intuitive eating, fosters healthy food and body relationships, and includes principles like honoring hunger and fullness cues and making sure you feel satisfied at all meals and snacks.

Intuitive eating encourages internal guidance from your own body and mind (rather than external guidance like the number on the clock) and helps you reconnect to your innate ability to nourish yourself.
If you are struggling with an eating disorder, working with a treatment team can help you find the best eating pattern for you right now. That may be using a specific meal plan, the plate-by-plate-approach, or a different structure.
Eating intuitively in recovery usually takes time and intentional steps with professional guidance and support, and it usually happens later in recovery.
Here are a few general tips for finding balance in eating and building a positive relationship to food, which will support your overall mental and physical well-being:
- Eat every few hours during the day, by starting with breakfast and continuing with lunch and dinner and snacks in between meals as needed.
- Ensure you eat a balanced diet on a regular basis by consuming the three macronutrients: carbs, fats, and proteins.
- Leave room for “fun foods,” or less nutrient-dense foods that you enjoy. (Cake, anyone?).
- Remember your needs can change from day to day, and that’s okay.
Keep in mind that if you’re in early recovery, or have specific nutrition needs or concerns, working with a registered dietitian is helpful.
The bottom line
Intermittent fasting may be trendy and flashy, but its alleged benefits are not based on solid evidence. And it carries several risks that can seriously harm your physical and mental health.
Additionally, intermittent fasting can lead to disordered eating behaviors or even an eating disorder. The healthiest choice is to prioritize your holistic well-being, which can’t be found in any restrictive diet or eating pattern.
If you or someone you love is struggling with disordered eating or rigid food rules that are interfering with health and the ability to live a full life, help is available. Speak to your medical provider or schedule a consultation with an Equip team member.
FAQ
Who should avoid intermittent fasting?
Some people should avoid intermittent fasting. These include people with a current or past eating disorder or disordered eating behaviors, children and teens, people who are pregnant or breastfeeding, and people who experience gallbladder attacks. Additionally, people who have diabetes should consult their clinicians to see whether intermittent fasting is safe for them.
Is skipping meals the same as intermittent fasting?
No, skipping meals and intermittent fasting are not the same thing. Intermittent fasting typically involves a feeding window and a fasting window during a 24-hour period, though other fasting schedules also exist. Many people doing intermittent fasting schedule their fasting window so that the bulk of it is during the night. Because of this, they may skip having a morning meal to extend their overnight fast. Alternatively, some people skip dinner as part of the process.
Why is intermittent fasting so popular right now?
Intermittent fasting is so popular right now because it has become a dieting trend. You do not need to fast, however, to manage health or weight.
Can intermittent fasting delay eating disorder recovery?
Yes, intermittent fasting can delay or complicate eating disorder recovery. This is because the dieting method relies on external cues, such as the clock, rather than your body’s hunger and satiety cues, to determine when you should eat or when you’re satisfied. It can exacerbate bingeing and restriction behaviors and worsen an existing eating disorder.
Catterson, James H et al. “Short-Term, Intermittent Fasting Induces Long-Lasting Gut Health and TOR-Independent Lifespan Extension.” Current biology : CB vol. 28,11 (2018): 1714-1724.e4.
Ganson, Kyle T et al. “Intermittent fasting: Describing engagement and associations with eating disorder behaviors and psychopathology among Canadian adolescents and young adults.” Eating behaviors vol. 47 (2022): 101681. doi:10.1016/j.eatbeh.2022.101681
Mitchell, Sarah J et al. “Daily Fasting Improves Health and Survival in Male Mice Independent of Diet Composition and Calories.” Cell metabolism vol. 29,1 (2019): 221-228.e3.
Patterson, Ruth E et al. “Intermittent Fasting and Human Metabolic Health.” Journal of the Academy of Nutrition and Dietetics vol. 115,8 (2015): 1203-12.
Shin, Bae Kun et al. “Intermittent fasting protects against the deterioration of cognitive function, energy metabolism and dyslipidemia in Alzheimer's disease-induced estrogen deficient rats.” Experimental biology and medicine (Maywood, N.J.) vol. 243,4 (2018): 334-343.
Varady, Krista A et al. “Clinical application of intermittent fasting for weight loss: progress and future directions.” Nature reviews. Endocrinology vol. 18,5 (2022): 309-321.
Welton, Stephanie et al. “Intermittent fasting and weight loss: Systematic review.” Canadian family physician Medecin de famille canadien vol. 66,2 (2020): 117-125.







